This care process model helps guide the general practitioner on outpatient screening and management of type 2 diabetes in patients within the University of Utah Health and Intermountain Healthcare systems. It was created by general pediatricians at the University of Utah School of Medicine and reviewed by pediatric endocrinologists at Primary Children’s Hospital. It is based on recommendations from the Intermountain Healthcare Pediatric Diabetes Care Process Model and the American Diabetes Association [American: 2021]. In 2023, it was updated to incorporate screening guidelines from the American Academy of Pediatrics Clinical Practice Guideline for the Evaluation and Treatment of Children and Adolescents With Obesity [Hampl: 2023].
Its purpose is to empower the general practitioner to screen for and manage pediatric type 2 diabetes while providing guidance about escalation of care and referral to diabetes specialists. Using the care process model will help primary care clinicians avoid delays in treatment while awaiting specialty consultation and reduce unnecessary referrals.
Key Points
1. Patients with BMI ≥95th% percentile for age and sex who are ≥10 years old or pubertal should be screened for type 2 diabetes with a fasting plasma glucose or a HgbA1c.
2. Patients with BMI ≥85th% to <95th% percentile for age and sex with ≥1 diabetes risk factors who are ≥10 years old or pubertal should be screened for type 2 diabetes with a fasting plasma glucose or a HgbA1c.
3. Patients with obesity, pre-diabetes, and type 2 diabetes should be treated with lifestyle and dietary interventions.
4. Patients diagnosed with type 2 diabetes should be initiated on metformin therapy as long as no contraindications exist.
5. Patients with HgbA1c in the 6 – 6.4% range or with continued impaired glucose tolerance after 6 months of lifestyle interventions may be started on metformin.
6. If fasting plasma glucose or HgbA1c places the patient in the diabetic range, perform recommended lab work to help rule out diabetic ketoacidosis (DKA) and type 1 diabetes.
7. Patients with DKA should be emergently referred to a facility with pediatric resources for DKA management.
8. Consider adding a GLP-1 agonist in patients with continued HgbA1c elevation and impaired glucose tolerance after starting metformin.
9. If considering insulin therapy, consult or refer to pediatric endocrinology.
Pediatric Type 2 Diabetes Care Process Model
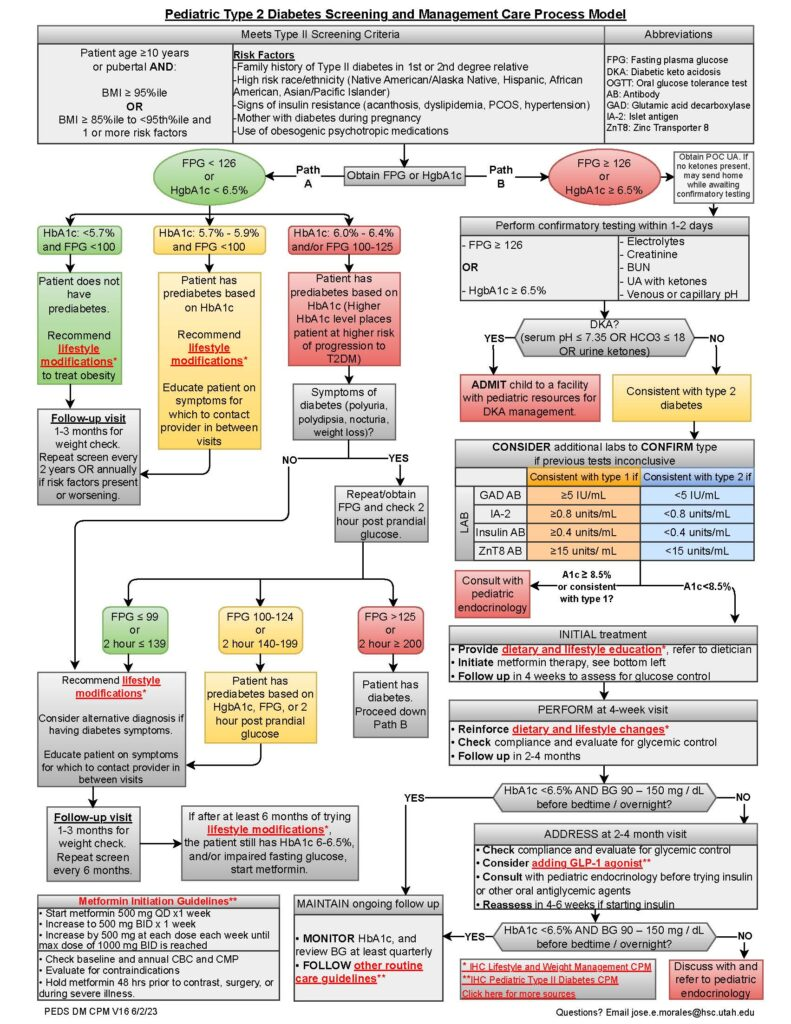
Click the Care Process Model image above to enlarge. Please note that on the algorithm phrases in bolded, red text link to Intermountain Healthcare’s Pediatric Clinical Program’s “Diagnosis and Treatment of Pediatric Type 2 Diabetes” and “A Primary Care Guide to Lifestyle and Weight Management for Children and Adolescents” care process models and provide further guidance on each topic.

Lifestyle and Weight Management for Children and Adolescents (Intermountain Healthcare) care process model

Diagnosis and Treatment of Pediatric Type 2 Diabetes (Intermountain Healthcare) care process model
Referrals
- Pediatric Endocrinology
- Diabetes Clinics
Tools
Page Bibliography
American Diabetes Association. (2021). 13. Children and Adolescents: Standards of Medical Care in Diabetes-2021. Diabetes Care, 44(Suppl 1), S180–S199. https://doi.org/10.2337/dc21-S013
Hampl, S. E., Hassink, S. G., Skinner, A. C., Armstrong, S. C., Barlow, S. E., Bolling, C. F., Avila Edwards, K. C., Eneli, I., Hamre, R., Joseph, M. M., Lunsford, D., Mendonca, E., Michalsky, M. P., Mirza, N., Ochoa, E. R., Sharifi, M., Staiano, A. E., Weedn, A. E., Flinn, S. K., … Okechukwu, K. (2023). Clinical Practice Guideline for the Evaluation and Treatment of Children and Adolescents With Obesity. Pediatrics, 151(2), e2022060640. https://doi.org/10.1542/peds.2022-060640
Article History
The Medical Home Portal last published this article in June 2023. Topical Reviews in Pediatrics (TRIP) reprinted it in November 2024. The Medical Home Portal, retired in July 2024, provided diagnosis and management information for pediatric conditions, guidance for immediate steps after a positive newborn screen result, and in-depth family education to improve outcomes for children with complex medical care needs.
The full archive can be found at the Medical Home Portal Archive.
Topical Reviews in Pediatrics (TRIP) includes archival and updated content from the Medical Home Portal and features new, contemporary topics in pediatrics.
Initial publication: December 2021; last update/revision: June 2023
- 2023 revision: Jose Morales Moreno, MDA, Carole H. Stipelman, MD, MPHA, Allison Smego, MDA
- 2022 revision: Jose Morales Moreno, MDA, Carole H. Stipelman, MD, MPHA, Allison Smego, MDA
- 2021 revision: Jose Morales Moreno, MDA, Carole H. Stipelman, MD, MPHA, Allison Smego, MDA
AAuthor; CAContributing Author; SASenior Author; RReviewer

